AONN+ Blog
Top 3 Takeaways from December’s Facebook Live Event: “State of Clinical Trials and the Role of the Navigator”
By Rosie Kelly
The state of clinical trials has been impacted by the COVID-19 pandemic. In December’s Facebook Live event, experts highlighted the integral role of the navigator in providing assessment, education, and support for patients with cancer who are considering their clinical trial options.
The Impact of COVID-19 on Advocacy Organizations
The COVID-19 pandemic has financially impacted organizations that have provided support for patients with cancer.
The Affordable Care Act and the Cancer Community
By Rosie Kelly
The Affordable Care Act is being reviewed by the Supreme Court. Cancer organizations, including AONN+, provide an infographic to help patients with cancer understand the potential implications of the law being repealed.
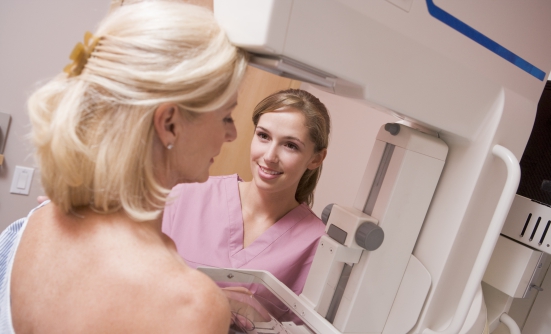
Reinstating Cancer Screenings for All Patients
Cancer screenings have been delayed due to the COVID-19 pandemic, but patients are now running the risk of missing a cancer diagnosis or receiving a higher stage diagnosis.
Top 3 Takeaways from November’s Facebook Live Event: “Equipping Patients, Family Members, and Caregivers at the Holiday Season”
By Rosie Kelly
The holidays are an especially stressful time for those dealing with a cancer diagnosis. In November’s Facebook Live event, experts discussed ways for oncology nurse and patient navigators to help equip their patients, family members, and caregivers deal with holiday stress and the new normal of COVID-19.
An Update on the Commission on Cancer’s Recent Accomplishments
AONN+ representative Lillie Shockney provides an update on the Commission on Cancer (CoC) annual plenary meeting that was held virtually this year.
Takeaways from Episode 4 of the Heart and Soul of Oncology Navigation Podcast: Professional Development and the Role of Certification
By Rosie Kelly
In episode 4, oncology navigators from different specialties explore how professional development and certification have helped them be a better navigator for their patients.
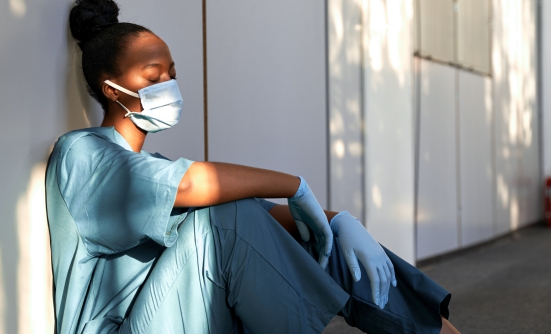
Daily Struggles of Oncology Navigators
By Rosie Kelly
Oncology navigators face new challenges every day. Becoming an AONN+ member means receiving resources and access to a community that addresses the needs of every kind of navigator.
Race and America: How Medicine Earned the Mistrust of Americans
Oncology navigators are often charged with addressing health disparities. The history behind these disparities has led to a deep mistrust between disparate populations and medicine.
Takeaways from Episode 3 of the Heart and Soul of Oncology Navigation Podcast: Challenges with Disparate Populations
By Rosie Kelly
Linda Burhansstipanov and Linda Fleisher focus on cultural humility and the health disparities that exist among different cultures in episode 3 of the AONN+ podcast.
Thank You to Our Corporate and Alliance Partners!

Advocating Partner

Supporting Partner

Supporting Partner

Supporting Partner

National Alliance Partner

National Alliance Partner

National Alliance Partner

National Alliance Partner
Privacy Notice | Terms of Use
© 2009- DBA AONN+ Academy of Oncology Nurse & Patient Navigators® | 15 W 38th St. Ste 1209, New York, NY 10018-5501 |
AONN+ DBA AONN+ is a 501(c)(6) organization under federal tax guidelines. AONN+ Foundation for Learning, Inc. a 501(c)(3) organization under federal tax guidelines.
AONN+ Advantage, LLC, a wholly owned subsidiary of AONN+.