The 2021 Virtual Midyear Conference was held May 13-16, with 2 optional preconference programs offered on May 12. The conference was again held virtually on our interactive digital platform. Live programming followed the format that was employed during the past 2 conferences—with excellent results. As attendees and presenters have become more familiar with the virtual format, the opportunities for communication and engagement have expanded.
And of course, this meeting was packed with informative content and dynamic presenters in the general sessions and breakouts that members expect, and we added more moderated networking events to maximize the time investment in every facet of the meeting. Attendees tell us that they love the opportunity to connect with expert faculty and navigators from around the world as well as with AONN+ leadership through these interactive features.
Preconference Sessions Offered Opportunities for In-Depth Exploration of Selected Topics
Prehab/Rehab
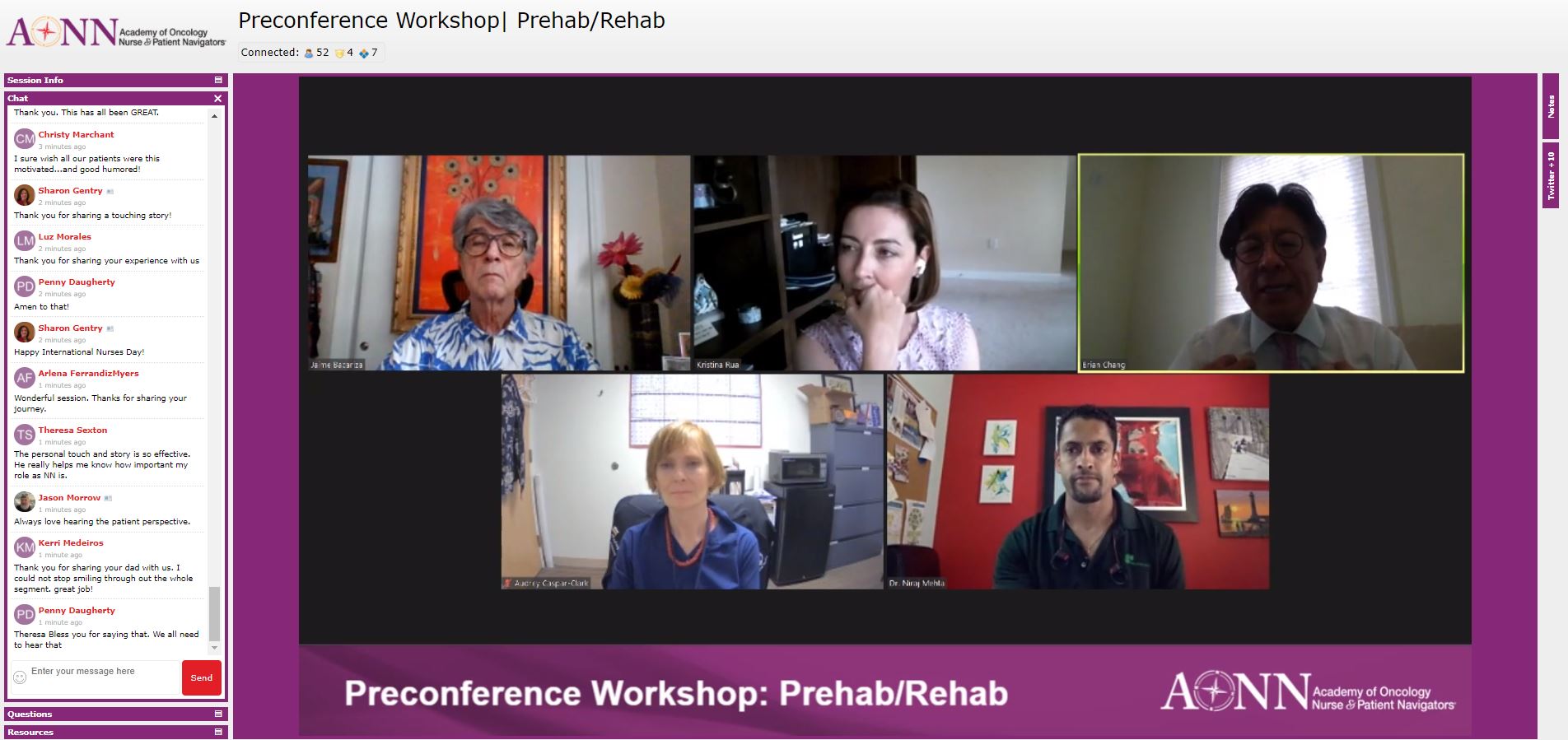
In this workshop, presented by Adrian Christian, MD, MHCM; Joy C. Cohn, PT, CLT-LANA; Jaime Bacariza; Niraj Mehta, MD; Brian M. Chang, DDS, FACP, FAAMP; Audrey Caspar-Clark, MA, RDN, LDN; Amy Sides, DPT, CLT-LANA; Kristin M. Carroll, PT; and Nicole Dugan, facilitators and attendees discussed how employing prehabilitation and rehabilitation best practices can strengthen a cancer-care program as well as meet the survivorship requirement of the Commission on Cancer.
The first part of the workshop focused on definitions of prehabilitation and rehabilitation and explored how such programs can be developed and administered. As the panelists explained, prehabilitation is an evidence-based process that occurs in the time between diagnosis and the start of acute care, while cancer rehabilitation deals with helping patients overcome side effects that may occur due to chemotherapy treatment and other interventions.
The panel drew from a wide range of specialties, and each participant discussed how a patient’s quality of life may be improved through different therapeutic techniques or processes.
The Nuts and Bolts of Building a Navigation Program
This intensive seminar offered a primer on the elements necessary for building a navigation program or for improving an existing one. The session was led by experts in various aspects of navigation, including members of the AONN+ leadership team. Kristina Rua; Tricia Strusowski, MS, RN; Chelsea Passwater, MSN, RN, AGCNS-BC, OCN; Megan Solinger, MHS, MA, OPN-CG; Zarek Mena, OPN-CG; Michelle Hubert-Fiscus, MSN, RN; Rowan Robinson, MSc, PGDip, N Ed, PGDip ONS, RN; Kym Dean, RN, BSN, OCN; and Emily Gentry, BSN, RN, HON-ONN-CG, OCN, called on their individual knowledge of specializations and navigation fields to present a truly comprehensive overview of the crucial factors involved in creating a successful and sustainable navigation program.
Topics presented included an exploration of current best practices and the application of real-world knowledge; identification and utilization of metrics outcomes; and the scope and responsibilities of licensed and unlicensed navigators in a collaborative and multidisciplinary program. New and newly expanded technologies, such as telehealth, were also discussed. Navigators learned strategies for measuring and communicating their worth to administrators and other stakeholders in the oncology space. In breakout sessions, participants rolled up their sleeves and interacted with experienced navigation program leaders to ask questions, strategize, and examine creative ways of facing current and ever-changing challenges.
Official Conference Kickoff!
As usual, the conference kicked off with greetings and messages from Academy leadership. AONN+ Co-Founder Lillie Shockney welcomed attendees with her customary warmth and enthusiasm. She was followed by other members of the leadership team—Penny Daugherty, Monica Dean, Emily Gentry, and Peg Rummel—and Lisa Hartman, MS, MA, BSEd, BSN, RN, was introduced as the new Director of Certification, AONN+ Foundation for Learning. It was wonderful to see familiar faces and to greet new attendees! Their special messages included an appeal to all members to consider sharpening their skill set and deepening their involvement in AONN+ by becoming involved in committee work. Details about the upcoming certification exams were announced, with dates and locations.
In her much-anticipated welcome statement, AONN+ Program Director Sharon Gentry took a few moments to address the difficult circumstances of the past year and commended navigators for the ways in which they have risen to face the challenges—both personal and professional—of 2020 and beyond. As always, the opening remarks from AONN+ leaders set the stage for the events to come, helped build excitement, and framed a sense of mission and purpose for all attendees.
The day’s program of full-length general sessions was incredibly well received, and attendees had abundant opportunities to weigh in with questions and comments, both during an active live chat forum and in moderated question-and-answer periods following the presentations. A look at the agenda shows the breadth and depth of the topics covered during this conference. Panels that focused on geriatric issues in cancer care, practices and problems in electronic record systems, and dimensions of financial navigation offered actionable information and techniques in rich and compelling sessions.
Making a Business Case for Financial Navigation
This panel, presented by Angie Santiago, CRCS, Dan Sherman, MA, LPC, and Clara N. Lambert, BBA, OPN-CG, delved into the many aspects to consider in creating and running a financial navigation program. Research has shown that financial navigators contribute to patient satisfaction and the reduction of financial toxicity. The panelists offered some truly eye-opening examples and statistics that showed how important it is for informed and committed financial professionals to be involved in the navigation project. Panelists explored the types of credentials that financial navigators typically earn and discussed the journey to becoming a financial navigator. They also provided case studies in which they outlined how a well-informed financial navigator can nimbly negotiate the complex maze of programs such as Medicare—resulting in cost-savings that will benefit the patient and contribute to a more positive patient experience. In addition, they discussed practical aspects of financial navigations to the overall administration of healthcare and presented ways to maximize and demonstrate financial return on investment for programs that employ a financial navigator.
Leveraging Technology to Enhance Navigator Workflow and Metrics Collection

Utilizing a question-and-answer format throughout the panel, Christina Payne, RN, MSN, OCN, Jessica MacIntyre, APRN, NP-C, AOCNP, and Zilipah Cruz, RN, MSN, tackled the complexities of EMR systems large and small through the specific lens of their own experience and their hands-on expertise in administering programs that have adopted EMR systems. Acknowledging the wide variety in the size of cancer-care programs, the types of EMRs used, and the degree of technological savvy possessed by users of current EMRs, the panelists fielded a comprehensive series of questions. Among the topics they discussed were workflow, team communication, and quality improvement initiatives. They also explored EMR capabilities and the pros and cons when it comes to tracking navigation workflow and metrics. The panelists shared many of their real-world data and presented best practice examples with techniques focused on initiating changes.
Geriatric Oncology

Using oncology care to create clinically relevant illustration and case studies, Sarah Kagan, PhD, RN, AOCN, APRN-BC, FAAN, FGSA, offered solutions that can be employed through person-centered, age-friendly models of care.
In this session, Dr Kagan defined some of the major concepts in person-centered, age-friendly models of care and presented ways to integrate these concepts into daily clinical practice. She explained that these goals have been created in relation to other national and international initiatives.
Moving beyond simplistic definitions of ageism as “elder bashing,” Dr Kagan provided examples to show how ageism can be reflected through even seemingly positive interactions. In addition, she explained the ways in which ageism combines with other forms of discrimination to negatively impact the overall healthcare outcome for patients who experience multiple and intersecting forms of discrimination.
This presentation was filled with Dr Kagan’s clinical pearls and insights, and she presented many actionable tips for combating discriminatory practices with a practical outline for making changes.













